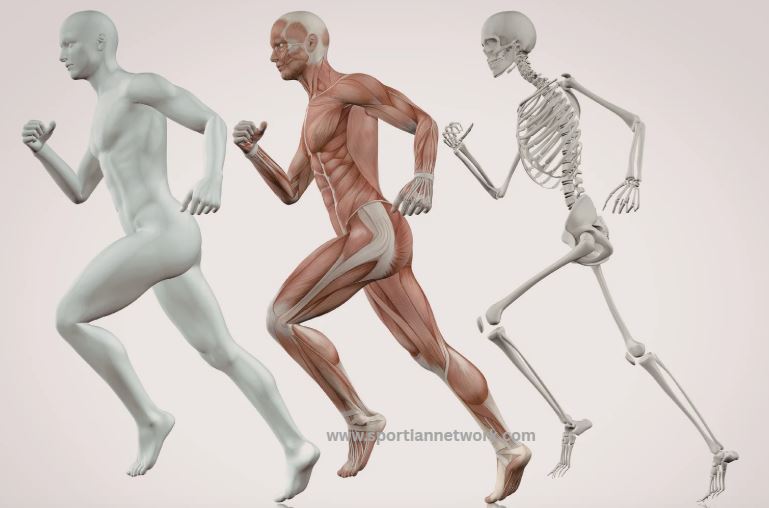
Bone is not static tissue. It remodels constantly throughout life in response to the mechanical demands placed on it. This is the most important thing to understand about bone density and exercise, and it is also the fact most athletes never learn. The skeleton you have at 40 is largely the product of the loads you placed on it at 15, 20, and 25, but the loading you do now still matters considerably and always will.
This article covers the biology of how bone responds to exercise, which training methods build the most bone, which sports leave athletes surprisingly vulnerable, and what nutritional factors interact with the training stimulus.
How Bone Adapts to Mechanical Load
Bone tissue contains specialised cells called osteoblasts and osteoclasts. Osteoblasts build new bone matrix. Osteoclasts break it down. In healthy, well-loaded bone these two processes are in balance, and when loading increases the balance tips toward formation. When loading decreases or is absent, it tips toward resorption and bone mineral density falls.
The stimulus for bone formation is mechanical strain, the degree to which bone tissue deforms under load. When strain exceeds the habitual level the skeleton is accustomed to, bone cells detect this through a process involving fluid movement in tiny channels within the bone structure. This triggers osteoblast activity and new bone is laid down in the direction and magnitude of the applied load. This is why the dominant arm of a tennis player has measurably greater bone density than their non-dominant arm, and why the tibias of sprinters are denser than those of non-athletes.
The Wolff’s Law Principle in Practice
The long-established observation that bone adapts to the forces placed upon it is commonly called Wolff’s Law. The practical implication is that bone responds specifically to the type of load applied. Compressive forces from weight-bearing activity produce different adaptations in different skeletal regions than bending forces from impact or torsional forces from rotational sport. You cannot build hip bone density with wrist exercises. The adaptation is local to the loaded region.
This specificity matters enormously for programming. An athlete who trains exclusively in the pool or on a bike is loading their cardiovascular system and muscles without loading their skeleton in ways that drive meaningful bone formation. Their fitness can be excellent while their bone density lags behind a less aerobically capable athlete who runs and lifts.
Which Types of Exercise Build the Most Bone
Not all exercise produces the same skeletal stimulus. The key variables are magnitude of load, rate of load application, and novelty of the loading pattern.
High-Impact Weight-Bearing Activity
Running, jumping, and landing activities produce ground reaction forces that can be two to five times body weight through the lower limbs. These forces, applied repeatedly across training sessions, provide a powerful stimulus for bone formation in the hip, femur, tibia, and calcaneus. Sprinting and jump-heavy sport produce larger strain magnitudes than steady-state jogging, which means sprint athletes typically have greater lower limb bone density than distance runners for the same training age.
Plyometric training is among the most osteogenic activities available to athletes. The rapid loading and unloading cycle of jump landings creates high-strain-rate stimuli that are particularly effective at driving bone adaptation. Our article on plyometric training for athletes covers how to structure jumping and landing work progressively, and the bone adaptation benefits are a genuine secondary gain from training that is primarily programmed for power development.
Resistance Training
Heavy compound lifting loads the skeleton compressively through the spine, hips, and long bones of the lower limb in a way that running does not fully replicate. Squats, deadlifts, and loaded carries apply forces through the axial skeleton that are highly osteogenic for the vertebrae and proximal femur, which are the regions most relevant to long-term fracture risk and osteoporosis. An athlete who runs but never lifts builds good tibial and calcaneal density but may underload the spine and hip.
The load must be meaningful. Light resistance training does not produce the same bone stimulus as heavy loading. Research consistently shows that training at 70 to 85 percent of one-rep maximum or above produces significantly greater bone adaptation than the same volume at lower intensities. This is one reason progressive strength training, not just general physical activity, is the appropriate recommendation for athletes who want to maximise their bone density. Our posterior chain training guide covers the compound lower body movements that load the skeleton most effectively, and the trap bar deadlift is a particularly useful tool for athletes who want high spinal and hip loading with lower technical demand than a barbell deadlift.
Multidirectional and Novel Loading
The skeleton adapts most strongly to loading patterns it has not previously encountered. This is why athletes who only perform one type of training reach a plateau in bone adaptation faster than those who vary their loading patterns. Lateral movements, rotational forces, and multidirectional impact all stress the skeleton in planes that straight-line running and bilateral lifting do not cover. Sports like basketball, soccer, and rugby that involve frequent changes of direction and unpredictable loading patterns produce higher whole-body bone density than sports with more uniform movement demands.
For athletes whose sport involves primarily linear loading, incorporating lateral jumping, rotational medicine ball work, and single leg training adds novel loading planes that drive continued bone adaptation rather than allowing accommodation to a repetitive stimulus.
Sports That Leave Athletes Bone Vulnerable
Some of the fittest athletes on the planet have surprisingly poor bone density. Understanding which sports create this paradox is important for coaches and athletes in those disciplines.
Swimming
Swimmers are among the least osteogenic athletes in terms of skeletal loading. Water provides buoyancy that offloads body weight, so the ground reaction forces that drive bone formation in land-based sport are absent entirely. Elite swimmers typically have lower bone mineral density than athletes in impact sports despite training volumes that would suggest exceptional fitness. This does not make swimming a poor training choice, but it does mean swimmers who do not supplement their training with land-based impact or resistance work are accumulating a skeletal deficit that becomes relevant as they age.
Cycling
Road cyclists face a similar issue for similar reasons. Seated pedalling loads the lower limbs against the pedal but does not produce meaningful ground reaction forces through the hip and spine. Studies of competitive cyclists, including professional road racers, consistently show lower spinal bone density compared to age-matched controls who engage in weight-bearing activity. Cyclists who combine their riding with running or lifting offset this risk. Those who train almost exclusively on the bike do not.
Endurance Running at High Volume
Distance running is weight-bearing and does produce a bone stimulus, but very high training volumes combined with caloric deficit and low body weight create conditions that can undermine bone health even in athletes who are running regularly. The bone stimulus from running is moderate compared to high-impact sports. When energy availability drops below the threshold needed to support bone remodelling alongside training demands, the osteogenic effect of the running disappears and bone density falls. This is particularly relevant in female distance runners and connects directly to the Relative Energy Deficiency in Sport picture.
The Peak Bone Mass Window
Bone density is not equally trainable at all ages. Peak bone mass is achieved somewhere between the late teens and mid-twenties, with approximately 90 percent of adult bone mass accumulated by age 18 in most individuals. The decade of adolescence and early adulthood is the period during which skeletal investments pay the highest returns.
This has direct implications for youth athletic development. Loading the skeleton appropriately during adolescence through sport participation and resistance training builds a higher peak bone mass that provides a larger reserve against the age-related bone loss that begins in the fourth and fifth decades. An athlete who reaches peak bone mass with a dense skeleton starts their long-term decline from a higher baseline, which translates to meaningful protection against fracture and osteoporosis decades later.
Our article on strength training for teenagers covers appropriate programming for adolescent athletes, and the bone density benefit is one of the clearest long-term reasons to introduce resistance training early rather than waiting until adulthood.
Bone mass does not stop responding to loading after the peak is reached. The capacity for bone formation decreases with age but does not disappear. Adults who begin strength training in their thirties, forties, and beyond still produce measurable improvements in bone density at loaded sites. The gains are smaller than what is possible during adolescence, but the alternative of doing nothing produces guaranteed loss, which makes any loading stimulus worthwhile across the lifespan.
Nutrition and Its Interaction With Exercise-Induced Bone Adaptation
Exercise provides the stimulus for bone formation, but the raw materials must come from nutrition. Without adequate calcium and vitamin D, the osteogenic signal from training cannot be fully converted into new bone tissue.
Calcium
Calcium is the primary mineral component of bone matrix. Athletes with chronically low calcium intake have blunted bone responses to training stimuli regardless of how well their exercise programming is designed. Dairy products, fortified plant milks, leafy greens, and certain fish provide dietary calcium. The recommended intake for athletes is at least 1000 milligrams per day, with some evidence that bone-active athletes benefit from slightly higher intakes during periods of heavy training.
Athletes who restrict dairy without adequate calcium replacement from other sources are at particular risk. This pattern is common in athletes pursuing low body weight for aesthetic or performance reasons, where food restriction overlaps with specific avoidance of dairy, creating a dual deficit of energy and calcium that seriously undermines bone health.
Vitamin D
Vitamin D is essential for calcium absorption in the gut. Without adequate vitamin D, dietary calcium intake is largely wasted because it cannot cross the intestinal wall into circulation. Athletes who train primarily indoors, live at higher latitudes, or have darker skin pigmentation are at higher risk of vitamin D insufficiency. Blood testing is the only reliable way to confirm adequacy. Training load and sweat loss do not reliably indicate vitamin D status.
Athletes with confirmed insufficiency typically require supplementation to restore levels that support bone metabolism alongside the immune, muscle, and hormonal functions that vitamin D also regulates.
Energy Availability
The most important and most commonly overlooked nutritional variable for bone health in athletes is overall energy availability. When caloric intake is insufficient to cover both the metabolic cost of training and the baseline energy requirements of organ function, the body deprioritises bone remodelling as a non-essential process. Chronically low energy availability suppresses the hormones that drive bone formation, including oestrogen in female athletes and testosterone in male athletes, and elevates cortisol which promotes bone resorption.
This is the mechanism behind the bone density problems seen in lean sport athletes who chronically undereat. The exercise stimulus is present. The calcium may be present. But the hormonal environment created by low energy availability blocks the adaptive response. Our nutrition timing guide covers how fuelling around training affects recovery broadly, and ensuring energy intake is sufficient to support bone metabolism is part of the same picture.
Stress Fractures as a Bone Density Warning Sign
A stress fracture is a partial or complete fracture in bone that results from cumulative loading that exceeds the bone’s capacity to remodel and repair itself. They are not purely the result of overtraining in otherwise healthy bone. They frequently reflect bone that is less dense, less mineralised, or less structurally sound than it should be for the loading it is experiencing.
Athletes who develop stress fractures, particularly recurrent stress fractures or fractures at unusual sites, warrant investigation of their bone density, hormonal status, and nutritional history. Treating the fracture without addressing the underlying skeletal vulnerability allows the same pattern to recur.
Our article on shin splints covers the distinction between tibial bone stress reactions and soft tissue shin splints, which is an important diagnostic distinction because bone stress injuries require different management than muscle and fascial issues. Load management is central to both, which connects to the monitoring approach described in our session RPE guide.
Practical Programming Principles for Bone Health
Athletes who want to maximise bone health across a training career can apply a few consistent principles regardless of their primary sport.
Include high-load compound movements in the strength programme. Squats, deadlifts, and loaded carries applied progressively over months and years produce cumulative skeletal adaptations that nothing else matches for the spine and hip. This applies even to endurance athletes and swimmers who have no performance reason to lift heavy but have a strong longevity reason to do so.
Include some form of impact activity several times per week. For athletes whose sport is already high impact this is handled automatically. For cyclists and swimmers it requires deliberate addition of running, jumping, or sport-specific drills that introduce ground reaction forces the primary sport does not provide.
Vary the loading direction regularly. Lateral, rotational, and multidirectional movements drive bone adaptation in planes that sagittal-dominant training misses. Including single leg work, lateral jumping, and rotational strength exercises maintains novel loading stimuli and builds more complete skeletal density across the whole skeleton.
Protect energy availability consistently. No amount of appropriate exercise stimulus or calcium intake compensates for chronic low energy availability. Athletes in weight-sensitive sports should treat adequate fuelling as a non-negotiable component of bone health management alongside their performance nutrition strategy.
For female athletes specifically, the interaction between bone health, energy availability, and hormonal status is more acute and better studied than in male athletes. Our article on strength training for women athletes covers how training interacts with the hormonal environment in ways that are directly relevant to bone density management across different phases of the athletic career.